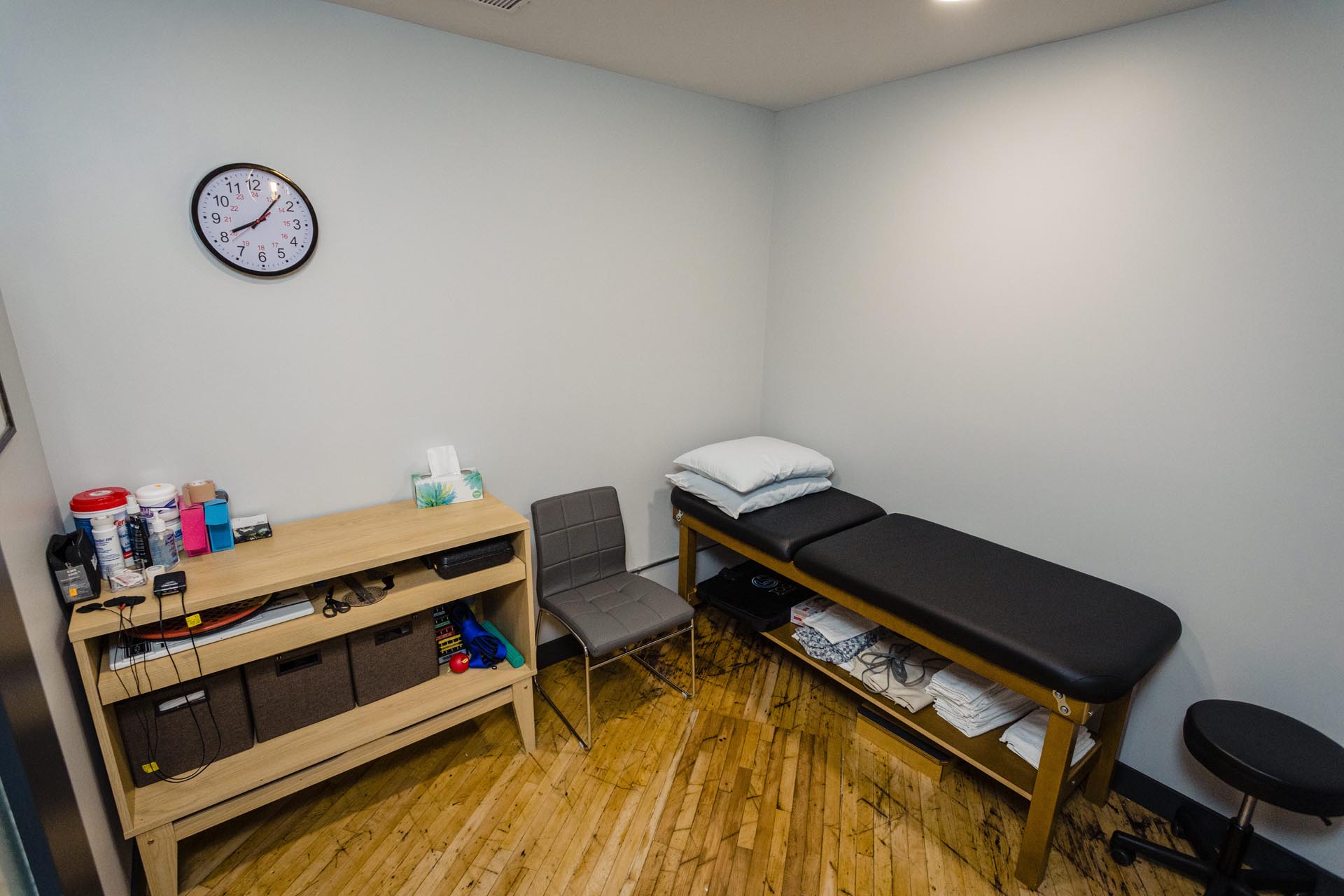
Pelvic Floor Physiotherapy
It is a misconception to think there is nothing you can do about urinary leakage. Research shows that physiotherapists with specialized training for the pelvic floor should be the first line of defence, before surgical consultation, for stress, urge and mixed incontinence in women. Pelvic floor physiotherapy cures or improves symptoms by decreasing the frequency and quantity of leaks, while improving symptoms and quality of life.
Our physiotherapist, Sarah Despatie, has completed multiple levels of certifications to become a pelvic floor physiotherapist. The pelvic floor is a network of muscles, fascia, and nerves that line the bottom of your pelvis and have many functions. When these muscles are not functioning properly, many conditions may arise. These include, but are not limited to: Urinary Incontinence, Stress Incontinence (SUI), Urge Incontinence (UUI), Mixed Incontinence (MUI), Functional Incontinence, Overflow Incontinence, Overactive Bladder (OAB), Pelvic Organ Prolapse (POP), rectocele, urethrocele, cystocele, enterocele, uterine prolapse, and vault prolapse. If you have any of these conditions or think you do, you may benefit from a physical therapy assessment of your pelvic floor.
Assessment:
The first time you meet with the physiotherapist, you will be able to discuss your symptoms and concerns, and goals you would like to achieve from treatment. Assessment of the pelvic floor musculature may include an internal exam to properly assess strength, tone or dysfunction. The patient is ALWAYS the priority, and if any client is not comfortable with an internal exam, other treatment options are available.
Treatment:
After meeting with the physiotherapist, an individualized treatment plan will be developed to help you reach your goals.
Treatment may include, but is not limited to:
-
Education
-
Behaviour Modification
-
Individualized Exercise Program
-
Stretching
- Strengthening Exercises
- Manual Therapy
- Muscular Stimulation
- Pain Relief & Control Techniques
Price List
Initial Visit:
| 60mins | $150.00 |
Follow-up Sessions:
| 30mins | $80.00 |
Concussion Therapy
Our three physiotherapists, Sarah Despatie, Hilary Veenstra and Christian Seguin, are certified concussion therapists, having completed specialized training to assess and treat concussions. Following a concussion, the “sitting in a dark room” approach is only effective for so long – in fact new research suggests that prolonged “black box therapy” is an ineffective technique in concussion management making this an out-of-date recommendation. Concussions, like other orthopedic injuries, should be properly managed and rehabilitated. While a certain amount of physical and cognitive rest is still the best approach in the early stages of the injury, having a health professional guide you through this step-by-step may prove to be invaluable. Sarah will conduct a thorough post-injury evaluation in order to gain a complete picture of your injury and how it’s impacted you.
This includes a detailed interview in order to obtain information on:
-
How the injury occurred
-
How you felt immediately after
-
How you’re feeling presently
-
History of previous concussions
- Current and past medical conditions
- Previous trauma/injury
- Current medications
The physical examination provides Sarah with insight into the severity of your injury, as well as specific impairments that may need to be addressed as part of an ongoing management strategy.
This portion of the testing may include a combination of the following:
-
Computerized neurocognitive testing
-
Balance testing
-
Strength and coordination testing
-
Screening of oculomotor skills
- Vestibular testing
- Gait assessment
- Orthopedic assessment of secondary injuries (eg. neck, back)
The assessment methods used are tailored to the immediate needs of the patient and Sarah will use her discretion on a case-by-case basis. (This information has been adapted from shiftconcussion.ca).
Price List
Initial Visit:
| 60mins | $120.00 |
Follow-up Sessions:
| 30mins | $80.00 |
Vestibular & Vertigo Rehab
The vestibular system is located in our inner ear and is a sensory system that provides us with our sense of balance and awareness of our orientation in space. Sometimes this system becomes affected and may result in symptoms of vertigo. Vertigo is not harmful, but presents as short, frequent and sudden sensations of spinning and dizziness. Sarah Despatie has received vestibular training, to assess and treat impairments of the vestibular system, such as vertigo.
Graston
Dr. MJ Cardinal has completed her M1, M2, and Graston Specialist certifications. Graston is an instrumented soft tissue mobilization technique directed at soft tissues to improve their tissue structure – whether it is chronic, acute or post- surgical. Graston technique uses instruments that enable the treatment of scar tissue and fascial restrictions during rehabilitation that allows for faster rehabilitation and with greater success when the goal is restoring range of motion, eliminating pain, and restoring normal function.
Cupping
Cupping is a form of alternative medicine in which cups are place on the skin and suction is created underneath. The therapist then glides the cups over the skin with the primary goal of breaking up restrictions in the fascia between the superficial skin layer and the muscular layer. Breaking up these restrictions helps to increase the range of motion, increase circulation which helps in muscular repair and decreasing pain.
Therapeutic Taping
Taping is used as a part of many treatment plans, and for many different injuries or conditions, to help relieve symptoms of pain, providing feedback to avoid painful positions and postures, and as a bracing effect to limit certain movements. Sarah Despatie uses many types of tape, such as athletic tape, leukotape, and kinesiotape, and Melissa Andre provides kinesiotape as an addition to her massage services.
Custom Orthotics
Through The Orthotic Group, Sarah Despatie has become a certified practitioner to perform gait analysis through biomechanical exams, the use of GaitScan technology, and foam casting in order to evaluate the need and benefits of custom orthotics for individual clients. Following a thorough assessment, Sarah will advise if you would benefit from wearing custom orthotics, place your order for custom orthotics, and make recommendations on shoe types.
Running Analysis
Sarah Despatie has completed training by The Running Clinic, and can apply this training to assess running biomechanics, apply running gait training interventions, recommend footwear for each individual runner, treat injuries from running or pain experienced while running, and help the runner return to their sport pain free.
Dry Needling
Sarah Despatie and Hilary have completed training to perform dry needling treatments. Dry needling is a treatment technique where a small needle, similar to those used in acupuncture, is inserted through the skin into a trigger point in a muscle. A trigger point is a taut band of muscle tissue, also known as a “muscle knot”. The goal of this treatment is to reduce pain, tension, and help improve your flexibility and movement.